What is PPE and How to Use it Correctly – Top Tips You Must Follow

Traditionally personal protective equipment (PPE) is used by healthcare workers, however, in recent times we’ve seen a significant increase of the general public using such equipment. PPE refers to the clothing or equipment designed to be worn by someone to protect them from risk of illness, this includes, eye goggles, face shields, face masks, gloves and gowns/suits. Using PPE effectively has become an important safeguard, but only one part, of protecting the wearer against potential infection. With the increase of PPE usage across the globe, it’s important people are aware of how to wear equipment correctly – because if worn incorrectly it may defeat the purpose of wearing it.
The World Health Organization advise on many ways to protect against potential infection. PPE is just one method and should be used in conjunction with frequent hand hygiene and respiratory hygiene (correct coughing etiquette).
Interestingly, in a recent study it was found 40% of healthcare workers make errors when removing PPE, significantly increasing the risk of spreading drug-resistant bacteria. This suggests, it is likely to be much higher for laypeople who haven’t had the training and simply buy equipment without educating themselves on how to use it. (Okamoto, K, Rhee, Y, Schoeny, M, Lolans, K, Cheng, J, Reddy, S, . . . Popovich, K, 2019). Additionally, another study revealed healthcare personnel contamination occurs due to failure to use PPE, PPE malfunction, incorrect use of PPE and self-contamination during care and during the removal process (Reddy, S, Valderrama, A, Kuhar, T, 2019).
With this in mind, it’s imperative people are aware of how to correctly put on and remove PPE to minimise the risk of infection.
Key Points to Know About PPE
- PPE is only one part of a system to protect against COVID-19 transmission.
- Hand hygiene is a foundational step before using any PPE.
- Appropriate use of PPE significantly reduces the risk of viral transmission and infection.
- Overuse of PPE is a form of misuse.
- Hand hygiene should always be performed before putting on an after removing PPE.
How to Use PPE Correctly
Especially during these uncertain times, it’s particularly important First Aiders understand the correct and incorrect use of PPE when providing First Aid to a patient.
Considering this, we’ve broken down how to correctly use each type of PPE and the common mistakes people make to ensure that you’re properly protecting yourself from potential infection.
Hand Sanitiser
Washing hands frequently or using alcohol-based hand sanitiser substantially reduces potential pathogens (harmful microorganisms) on the hands. Performing regular hand hygiene is considered a primary measure for reducing the risk of transmitting infection. Hand hygiene procedures include the use of alcohol-based hand rubs (containing 70% ethanol or 70% isopropanol) or hand washing with soap and water.
When to use Sanitiser
- All workers regardless of their role should use hand sanitiser if they’re unable to wash their hands:
- Before and after eating.
- Before and after smoking.
- After coughing or sneezing.
- After going to the toilet, and
- When changing tasks and after touching potentially contaminated surfaces.
How to use hand sanitiser
- Apply a 5-cent sized (1 pump) amount of hand sanitiser.
- Rub hands together covering all surfaces of hands and fingers, including palms.
- Rub in between fingers and around thumbs.
- Don’t forget your wrists and rub until hand sanitiser has dried.
What NOT to do
- DO NOT blow on your hands to make them dry faster.
- DO NOT use hand sanitiser as a substitute to washing hands.
- DO NOT use hand sanitiser more than 4 times in a row without washing hands.
Face Mask
Face masks are one of the most common pieces of PPE used to limit the spread of infection, including COVID-19. Masks can be used either for protection of healthcare workers (worn to protect oneself when in contact with an infected individual) or for source control (worn by an infected individual to prevent onward transmission). When providing First Aid, not all situations will present the need to wear a face mask, however, if at the risk of being exposed to bodily fluids and/or infection, face masks should be worn.
When to use face masks
- For those who may be unwell but are confirmed as negative when tested for COVID-19, so they do not spread cold or flu which may cause concern during a time of pandemic.
- When conducting CPR, as particles may be emitted during compressions.
The two most used face masks are the surgical mask and the N95. So, what’s the difference between the two? Well, surgical masks reduce the respiratory droplets from the wearer to others and the environment, they can also prevent the transmission of the virus from others to the wearer. Respirators (such as the N95) are specifically designed for healthcare workers where aerosol generated procedures are undertaken. Wearers need to be fit tested to ensure they are wearing the correct size (Q&A: Masks and COVID-19).
Surgical Mask
How to put on a surgical mask
- Perform hand hygiene.
- With clean hands, open the mask by the two straps. Ensure the white side of the mask is facing upwards.
- Place the straps over the ears and fit the mask so it’s securely over the chin and nose.
- Once positioned correctly, pinch the metal piece over the nose until secure.
How to remove a surgical mask
- Remove mask from two straps on either side of the ears.
- If contaminated, put mask into biohazard bag and into general waste. Dispose of mask in general waste if not contaminated.
- Perform hand hygiene.
N95 Mask
How to put on N95 mask
- Perform hand hygiene.
- With clean hands, open the mask by the two straps. Ensure the mask is securely fitted over the mouth and ears.
- Pinch the metal piece on the nose until securely in place and no air is coming through. Test the mask by inhaling in and out and checking for air leakage around the edges.
How to remove N95 mask
- Remove mask from two straps on either side of the ears.
- If contaminated, put mask into biohazard bag and into general waste. Dispose of mask in general waste if not contaminated.
- Perform hand hygiene.
What NOT to do
- DO NOT touch the surface of the mask when wearing or removing the mask
- DO NOT pull down the mask to talk to people
- DO NOT leave nose and mouth uncovered
What TO DO
- DO change the mask every 4 or so hours
- DO have the mask cover the nose and mouth
- DO change the mask if touched with unclean hands
Eye Goggles
Eye protection can act as a physical barrier from droplet spray and prevent unintentional rubbing of eyes between hand washing. For many instances, eye protection will not be required. Good hygiene practices should be followed if eye protection is used.
When to use eye protection
- When in potential exposure to any type of bodily fluid when interacting with someone who is unwell
How to put on eye goggles
- Perform hand hygiene.
- With clean hands, position goggles over eyes.
- Ensure the goggles are secure.
- Adjust fit if necessary.
How to remove eye goggles
- Remove goggles from straps.
- Wipe eye goggles with disinfectant wipes.
- Perform hand hygiene.
Coverall Disposable Suit
Suits with long sleeves are used to protect the wearers clothing from airborne droplets, which can then transfer on to hands and the face, or to others. Generally, coverall suits are not commonly used by non-healthcare workers.
How to put on PPE suit/gown
- Perform hand hygiene.
- With clean hands, put on face mask, eye goggles and gloves.
- Take PPE suit out of the bag and put on, leaving the zip open.
- Pull the hood over the head and zip up the suit.
- Fold and secure the zip cover, ensuring the suit is securely in place.
How to remove PPE suit/gown
- Unzip suit and remove hood.
- Gently pull the suit down, turning the suit inside out around the arms.
- Continue to roll down the suit to the ankles and then remove completely.
- Remove gloves, eye goggles and face mask. Put gloves, face mask, suit in a biohazardous bag and place in general waste.
- If wearing reusable goggles, wipe down with disinfectant wipes.
- Perform hand hygiene.
Gloves
Washing hands frequently or using alcohol-based hand sanitiser will usually be a better control measure against infection than wearing gloves. Importantly, the use of gloves does not replace the need for appropriate hand hygiene, which should be performed frequently. When a person wears gloves, they may come into contact with germs which are then transferred to other objects or their face if they don’t replace and dispose of or clean their gloves between tasks. Depending on the situation, gloves may be worn based on the risks and tasks to be performed.
When to use gloves
- When you’re unable to wash your hands or unable to access alcohol-based hand sanitiser.
- When providing first aid and/or medical treatment.
- When cleaning surfaces with sanitiser.
How to put on gloves
- Perform hand hygiene.
- With clean hands, put on one glove at a time.
How to remove gloves
- Pinch the outside of one glove. Do not touch bare skin.
- Peel the glove away from your body, pulling it inside out.
- Hold the glove you just removed in your gloved hand.
- Peel off the second glove by putting two fingers inside the glove at the top of your wrist.
- Turn the second glove inside out whilst pulling it away from your body, leaving the first glove inside the second.
- Put gloves into biohazard bag and into general waste if contaminated, if not put into general waste. Do not reuse the gloves.
- Perform hand hygiene.
What NOT to do
- DO NOT touch your face with gloves.
- DO NOT reuse gloves.
- DO NOT continue to use gloves if torn or damaged.
- DO NOT touch clean surfaces and/or items with contaminated gloves, e.g. mobile phones and car keys.
Medical Isolation Visor (Face shield)
Disposable face shields are PPE devices commonly used by many medical workers for protection of the facial area and associated mucous membranes (eyes, nose, mouth) from splashes, sprays, and spatter of body fluids. Face shields are commonly used as barrier protection for infection control against invisible pathogens. When providing first aid, face shields should not be used as a solitary face/eye protection, but rather as adjunctive to other PPE, such as protective face masks and goggles.
How to put on face shield
- Perform hand hygiene.
- With clean hands, pull strap over the head and fit so that the blue part is resting just above the eyebrows.
How to remove face shield
- Pull strap over the head.
- Dispose in general waste. If contaminated, put into biohazard bag and put into general waste.
- Perform hand hygiene.

It’s important to note PPE and other infection control methods work in conjunction with each other, such as continuing to perform hand hygiene while wearing a mask. More importantly, PPE worn incorrectly is just as dangerous as not wearing PPE, so taking extra steps to make sure equipment is worn and used correctly will help save lives.
With more TGA approved PPE now back on the market and accessible for individuals and workplaces to purchase directly, it’s time we all learn or update our awareness of best practice when wearing PPE.
- (2020). Rational use of personal protective equipment (PPE) for coronavirus disease (COVID-19).Available: https://apps.who.int/iris/bitstream/handle/10665/331498/WHO-2019-nCoV-IPCPPE_use-2020.2-eng.pdf. Last accessed 24th June 2020.
- Centres for Disease Control and Prevention. (2020). Respirator Trusted-Source Information.Available: https://www.cdc.gov/niosh/npptl/topics/respirators/disp_part/respsource3healthcare.html#:~:text=Is%20a%20surgical%20mask%20an,droplets%20including%20large%20respiratory%20particles.. Last accessed 24 June 2020.
- Okamoto, K., Rhee, Y., Schoeny, M., Lolans, K., Cheng, J., Reddy, S., . . . Popovich, K. (2019). Impact of doffing errors on healthcare worker self-contamination when caring for patients on contact precautions. Infection Control & Hospital Epidemiology, 40(5), 559-565. doi:10.1017/ice.2019.33
- Sujan C Reddy, Amy L Valderrama, David T Kuhar, Improving the Use of Personal Protective Equipment: Applying Lessons Learned, Clinical Infectious Diseases, Volume 69, Issue Supplement_3, 1 October 2019, Pages S165–S170, https://doi.org/10.1093/cid/ciz619
- World Health Organisation. (2020). Q&A: Masks and COVID-19.Available: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/question-and-answers-hub/q-a-detail/q-a-on-covid-19-and-masks. Last accessed 29 June 2020.
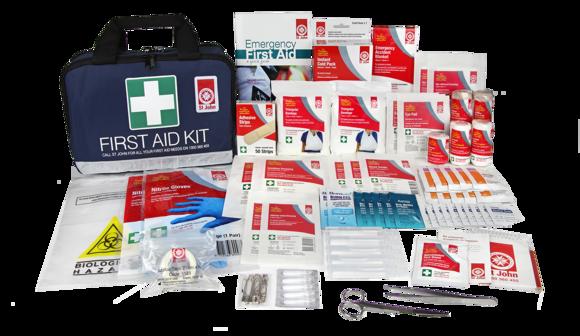
FIRST AID KITS, SUPPLIES & REFILLS
Being prepared with the right First Aid Equipment that is easily accessible and visible will reduce risks and response times in an emergency
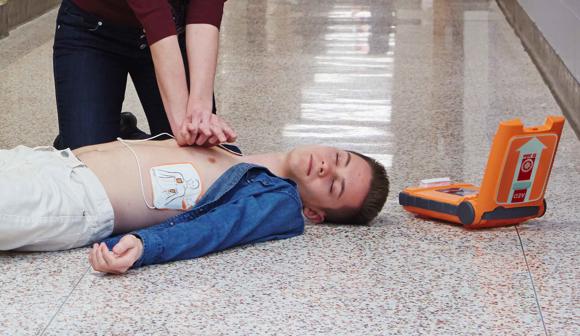
DEFIBRILLATORS
Having a defibrillator means you can step in with the tools to save a life before paramedics arrive – every minute counts. Research shows survival rates of up to 70% can be achieved if an AED is on hand.

CORPORATE PRODUCTS & COBRANDING
Partner with one of Australia's most trusted organisations to create a practical corporate gift for staff or clients

